The First Faculty Works on Improving the Quality of Teaching ... With the Help of Its Alumni
It is well known that medical competencies include three main areas: theoretical knowledge, practical skills, and communication abilities. Especially the second but in a sense also the third item were the main subject of discussions with our Faculty’s alumni. Aleksi Šedo, Dean of our Faculty, had recently with other members of the Dean’s College and student representatives met with representatives of a group of alumni who developed their own questionnaire to assess alumni views on the quality of teaching at the First Faculty of Medicine. Of course, one could object that the number of respondents was not quite representative, but the results were so interesting and important that Faculty management started to systematically try and respond to them.
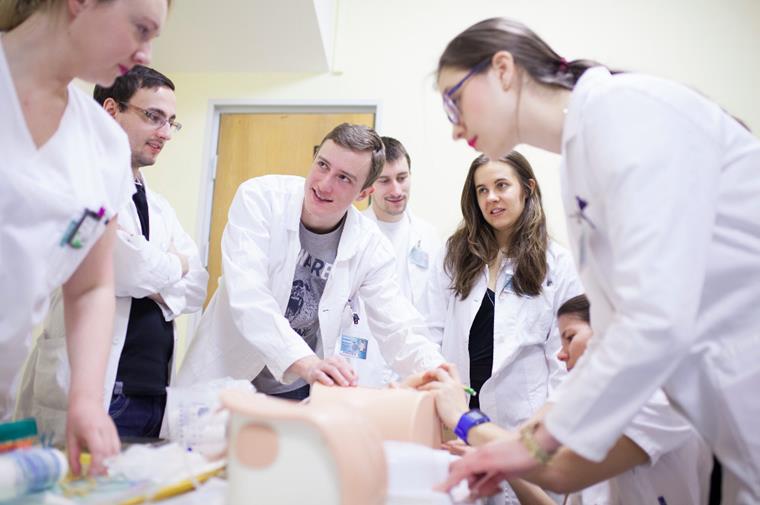
The meeting brought to light especially the alumni’s critical opinion of clinical instruction at the Faculty and its role in future performance of their profession. In particular, they noted lack of practical instruction during studies and subsequent shortcomings in practical skills at graduation. Discussions revolved around general directions in the development of medical teaching, which in our country tends to focus on broad theoretical foundations while practical skills are acquired mainly during pre-certification training.
In France, on the other hand, curriculum during the second half of undergraduate study has a more practical focus and medics are actively involved in the operation of hospitals as ‘externs’. After a while, they thus become thoroughly familiar with the foundations of administrative work, with differential diagnostic process, and ways of approaching actual therapy, which helps them feel better prepared for medical work. The disadvantage of this system is that there is not enough time in the programme to go through all areas of medicine in sufficient detail. There is no time to teach about rarer diseases and students do not have the opportunity to study some areas of clinical pathology. Regular work in a hospital can also take a lot of time that should be spent studying on one’s own. It would be best to combine the advantages of both systems and find a compromise where medics would be sufficiently familiar with the theoretical foundations of medicine on which they could build their clinical experiences, but also make sure that they are ready for medical practice.
Alumni came up with a number of concrete proposals that should help improve the situation. These proposals were discussed at the meeting, and now they are debated on the level of Faculty management, heads of clinics, and student representatives.
How to better organise the sixth year
Most discussed was the final, sixth year of study. Participants debated ways of improving the quality of instruction during internships that take place before the final examinations as well as organisation of the final year that would help better preparation for the state examinations (rigorosum examinations). Alumni proposed that, for instance, only subjects which are part of the state examinations be taught in the final year and that one or two weeks be reserved for preparation for these examinations. This is connected with the now debated extension of teaching into afternoon, which alumni claim would stretch into time which students should spend studying on their own. To increase the proportion of practical instruction, alumni suggest that compulsory clinical internships focused on patient contact be possible also in hospitals other than the General University Hospital and that for the entire or maximal possible part of duration of the internship. They drew attention to good experience which medical schools in Brno and Olomouc have with a system where their students must do their internships in ‘peripheral’ collaborating hospitals.
Alumni of the abovementioned Moravian medical schools were very happy with this system and emphasised its contribution to acquisition of necessary practical skills, especially because at external clinical institutions they came much more often in direct contact with patients. Another great advantage of the system is, in their view, that this way they repeatedly met with the most common medical issues within a clinical specialisation. In specialised university hospitals, this is rarely the case: students tend to meet with common ailments only in case of relatively severe complications.
What should be changed in the curricula
Many proposals had to do with the syllabus and scheduling. Among other things, the alumni were not satisfied with the way that subjects which later appear in the final examinations are split among a number of years, for instance gynaecology and internal medicine which are split between years five and six. In this context, there was a discussion about shifting the state rigorosum examination in internal medicine to year five. Another possibility would be adding some more time to paediatric medicine course, a time that could be used for introduction (if at all possible, not into lower years) and reconsider the volume of knowledge and skills required for the state rigorosum examinations. Based on their experience, the alumni find the current volume of requirements excessive. Yet because extension of time dedicated to any particular subject poses a difficulty, they propose that time be saved by merging the subjects Hygiene and epidemiology and Occupational medicine, which would moreover limit certain overlaps the curriculum.
The alumni appreciated the recently introduced e-learning course of X-ray diagnostics. They therefore propose that e-learning be used in theoretical instruction of some further clinical subjects, which could give students more time to spend at inpatient or outpatient departments and clinics. There was also a discussion about the need to improve communication between teachers and medics and eradicate situations which might lead to a feeling of disparagement or impression of lack of interest in study on the part of teachers and students, respectively.
Will the clinical base keep growing?
The management of our Faculty takes the proposals and comments coming from the alumni very seriously and started discussing them systematically in the Dean’s College in a ‘task force’ for clinical instruction and in a Committee for Assessment of Teaching. The two parties agree that clinical basis for medical teaching should be expanded. One of the reasons motivating this strategy if for instance the fact that thanks to development of knowledge and growing quality of current medical science, most diagnostic procedures have been moving to an outpatient mode, which tends to shorten the time patients spend in hospital. This is why students during their internships are unlikely to see the longitudinal development of disease in any particular patient. Moreover, the number of patients who do not wish to be examined by medics or in their presence is growing.
The Faculty is aware of possible benefits coming from securing further teaching hospitals, which is why, in collaboration with its task force and the committee on teaching activities, it has been monitoring and supporting an extension of instruction in clinical subjects at hospital beds outside the General University Hospital. At the moment, the degree of externalisation varies between various subjects and its provision is the responsibility of the chief guarantor of a particular subject. As part of updating of the curriculum, we can expect further diversification of clinical base for instruction in further clinical subjects taught in years four, five, and six. A concrete solution, that is, mainly a well organised selection of newly opened clinical teaching facilities, but unfortunately also overcoming of certain traditionalist views on the part of some teachers of clinical subjects, will require further discussions among experts. And by the way, the Faculty’s management has been encountering similar challenges also within the framework of the Erasmus student exchange programme. To wit, some university hospitals had been refusing to recognise teaching at other universities, including for instance courses at the prestigious Faculty of Medicine of the University of Heidelberg, as being of sufficiently high quality.
Will it be possible to unify teaching across faculties?
All participants in these discussions also agreed on the need to unify the content of courses and standards between teachers, institutes, departments, and medical schools on the basis of principles of evidence-based medicine. It is quite inappropriate when at examinations one teacher requires something different than another teacher or one teacher does not accept literature recommended by another teacher. This places students in a difficult situation where for some questions, they must learn various versions of responses and depending on the person of the examiner choose the correct one.
A solution might be found, at least to some extent, in creating updated teaching texts whose contents would be broadly agreed by persons teaching the subject in question. Even that, however, has been running into obstacles. Creation of suitable textbooks is difficult especially due to the speed of development in medicine. It is not always possible to publish a respected and generally supported textbook within the Faculty (and much less so to publish a text for several medical schools at once). The First Faculty of Medicine has been undertaking various steps but solution to this problem is unlikely to come quickly. Even so, some progress has been achieved and partial successes should be noted. In the case of subjects which appear in the state examinations, Faculty management has introduced unified lists of subjects to mastered for a particular subject. This should provide a starting point for our long-term goal, which is to achieve certain standards that must be met by all graduates of general medicine in the Czech Republic.
This is also why the First Faculty of Medicine has been the first medical school in the Czech Republic and Slovakia to propose at a meeting of all national and Slovak medical schools curricula of these subjects, which should serve as a source of inspiration for comparing with other medical schools’ curricula and invite various proposals of changes in terms of, for instance, the particular time spent on concrete subjects or the composition of various topics. Such changes are likely to take place at our Faculty soon as well. Particular possible changes will be discussed especially at meetings of the task force for clinical education. In order to promote emphasis on acquisition of clinical skills among our students, we introduced already in 2003 a logbook of mandatory procedures and meeting these requirements had become a standard condition of completion of studies at our Faculty.
Should medical simulations become part of the mandatory curriculum?
Various departments and institutes of the First Faculty of Medicine also offer opportunities to acquire further practical skills as part of optional medical procedures and support of extracurricular activities. The management emphasises the need to further develop modern simulator- and model-based teaching. This is the case of almost all institutes, but especially the Centre of Medical Simulations of the Institute of Physiology. It is planned that this mode of teaching will expand and in the context of ever shorter hospitalisations and lower willingness of patients to come in contact with the medics, it seems to be a suitable alternative to contact with real patients. Nevertheless, it seems that although due to the abovementioned reasons, which affect not only our faculty but medical teaching all over the world, simulator-based instruction is internationally becoming ever more important in the study of both clinical and preclinical subjects, students are not interested in it as much as we would have hoped. Although our SIM centre each year prepares a simulator-based course in practical solution of the most common acute conditions in medicine and this optional course is of a very high standard, its capacity is not at all filled. The management therefore plans to introduce medical simulations into the mandatory curriculum, whereby time for this would be found among courses whose contribution will be assessed as less significant.
Are students themselves likely to be more active?
Despite the Faculty’s efforts to address these challenges, it is clear that some comments and dissatisfaction of our alumni are well-founded. In part, one could prevent this situation by better communication with students. After all, students are represented in the Dean’s College, in the Academic Senate, and in the various work groups involved in continuous modifications of the curriculum. Faculty management expects that this representation is representative of the student body, functional, and that it actively contributes proposals for improvements. On the other hand, it is evident that students in the various organisation bodies of the Faculty represent only students still present at the school. This is why we miss, for instance, an important percentage of reactions especially to the final year and this important feedback is missing.
Views of the alumni are valuable also due to their perspective on how future physicians should be prepared for medical practice. This is something students are not in position to fully appreciate. The committee for assessment of teaching activities will therefore as soon as possible produce a plan of making feedback from alumni and sixth year students more efficient. We are also discussing further ways of improving and simplifying the current system, for instance by giving students an opportunity to evaluate teaching already during a course. To do that, however, we will have to address one crucial problem, namely a link between the evaluation system and the Student Information System, which is administered not by the Faculty but by the Charles University, i.e. centrally. It would have certain advantages, but the practical impact of this step must be further discussed and analysed.
Will alumni questionnaires become firmly embedded in our evaluation efforts?
The alumni poll complemented various efforts at improving the quality of teaching at the First Faculty of Medicine which have been already in progress and supported by the Faculty management as well as by the Committee for Evaluation of Teaching and the student chamber of the Academic Senate. On top of that, it brought in another perspective. It is to be hoped that this feedback from the alumni will help us identify new priorities and ways of improving teaching, especially clinical instruction.
It is clearly desirable that such polls take place among our alumni in future years as well. We would find out whether their statistical significance is growing, and it would give us a chance to compare progress from year to year. We are fully aware that feedback plays an extremely important role in setting the development of our Faculty on the right course as well as in preparing students of general medicine for their demanding future profession.
Tomáš Hanuš, Vice Dean for clinical education
Otomar Kittnar, head of Committee for Evaluation of Teaching
David Novotný, student representative
Photo: Veronika Vachule Nehasilová
