We Teach Non-Physicians to Better Understand Each Other
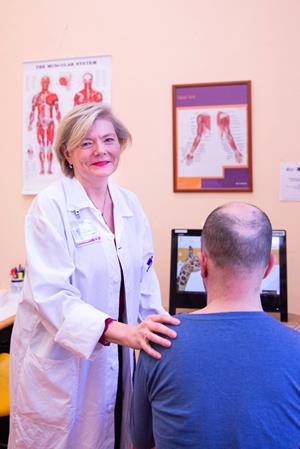
If she were to decide about her future today, she would, without a shadow of doubt, choose medicine again. While she was initially tempted by physiology, in the end, via a stop at neurology, she ended with rehabilitation medicine ... and she has no regrets. In her view, it is a medical specialisation with great future, an area whose full potential we are yet to fully appreciate. Her career has been linked to the First Faculty of Medicine from the outset and, as she herself admits, over time she gained here lots of experience with students, teaching, and with teachers who stand at the beginning of their career. This is also why she decided to run, for the first time, for a place in the Academic Senate of the First Faculty of Medicine. She was recently elected and what she sees it as her mission to work at improving connections between the theoretical and clinical departments and institutes at the Faculty and to support students’ school as well as extracurricular activities. MUDr. Yvona Angerová, Ph.D., Head of the Department of Rehabilitation Medicine.
What are the main things you would like to lobby for in the Academic Senate?
I believe there should be greater awareness of the non-clinical areas of medicine taught at our Faculty. Many people hardly know what people in these specialisations actually do. In addition to occupational therapists and physiotherapists, we of course also teach medics and I can see how the new generation is changing and what their demands of or comments on practical learning are. We should talk about it in the Senate and try to define shared goals. This is why I would like to establish closer links between the world of physicians and non-physicians: in rehabilitation, we are used to working as a team and if people start meeting already during their studies, it can have a positive impact on their future practice.
 You spent at the First Faculty already your school
years. How do you recall them?
You spent at the First Faculty already your school
years. How do you recall them?
I recall them very fondly, because during studies, one is young, and youth is fun to recall. I always liked the area of Karlov and Albertov, the clinics and institutes and departments and their historic buildings. During my studies, I also met many teachers who had a long-lasting impact on me, because their lectures were outstanding and from what they said, it was clear that their area of medicine is their hobby, not just their job. Throughout my studies, I used to go to the Institute of Physiology to Professor Pokorný to observe interneurons under a microscope. We even wrote a relatively successful article together, so I considered staying with physiology. In the end, however, I opted for practical medicine.
What provided the impulse that made you decide for rehabilitation medicine?
It was a bit of a coincidence. After maternity leave, I lost my neurologist post at the Bulovka Hospital and when deciding how and where to re-enter my profession, I liked an advertisement of the Department of Rehabilitation Medicine, which was looking for a doctor. Given the fact that this was a position at my alma mater, in an environment I liked, and moreover close to the Institute of Physiology, which I knew well, I decided to apply. And my application was successful. Over time, I found that rehabilitation is a very interesting area of medicine where I could certainly do quite a lot of work. And it turned out to be right, because that is where I stayed ...
… and for the past about a year, you have been heading it. How was that year?
The beginnings were incredibly hard. The situation we found ourselves in after the sudden death of Professor Švestková was extremely complicated. But gradually, many people started helping us, we regrouped and refocused, and found out that we simply have to function and do our best to continue in the work that had begun.
Why should students choose rehabilitation as their specialty?
I believe that this area of medicine has great future and is currently still rather underappreciated. Over the past two decades, rehabilitation medicine in our country had undergone many changes and its role is moving ever more towards urgent cases, for instance towards patients after stroke or brain trauma. But rehabilitation moves also into many areas other than neurology. We collaborate with orthopaedic surgeons, surgeons, plastic surgeons, pneumologists, but also general practitioners and paediatricians. We are often addressed even by colleagues from areas which may at first glance seem rather unlikely, such as dermatologists and their patients with systemic diseases. Modern technologies are also coming ever more to the fore. Ultrasound is nowadays used not only in therapy but also in diagnostics and in application of medications in joints and soft tissues. Rehabilitation offers plenty of opportunities for employment and people who enter this field can choose from a relatively wide range of further specialisations.
Should a rehabilitation specialist have any particular professional talents?
Like in many other areas of medicine, one of the most important things is communication with the patients and their families. Then one should also fully take into account the fact that rehabilitation medicine is really interdisciplinary, and it is therefore essential to respect other team members and listen to their views. Already Professor Pfeiffer, who founded our clinic, was one of the first persons to emphasise that rehabilitation includes not only medical professionals, but also social workers, teaching assistants, and numerous other non-medical professions. Naturally, a physician leads the team but in some cases, he or she need not be its most important part.
Do you think it is an advantage that you train your own non-physicians, that is, occupational therapists and physiotherapists?
I see that as an important priority. I was part of the effort that led to the establishment of occupational therapy as a specialisation which our Faculty was the first to offer a programme in within the Czech Republic. Within the framework of a large European project, we visited some other occupational therapy training centres which were part of healthcare schools, not medical faculties, and as a physician I saw that in these cases, courses in anatomy or physiology are on quite a different footing than at our Faculty. As physicians, we know why we need non-medical healthcare professionals, and this is also why we are in position to assess what these non-physicians should know when it comes to medicine. This helps our mutual communication and helps us form a more unified approach to the patient. I believe this is of a crucial importance. Our students of physiotherapy and occupational therapy definitely profit from the fact that their course takes place at a medical school.
Physiotherapy had won its place within healthcare a long time ago. How is occupational therapy doing in this respect?
Czech physiotherapy has a highly respected tradition and excellent foundations. When it comes to occupational therapy, whose main mission is to help patients be self-sufficient, help them return to normal life, many colleagues hardly know what it involves. The situation in occupational therapy is quite different, but I think that the adoption of the stroke programme helped us a lot. Thanks to it, a total of 45 stroke centres were established in the Czech Republic and each must include some inpatient rehabilitation unit with a resident occupational therapist. In my view, there are still too few occupational therapists, because as it becomes better known what their work is about, demand for these specialists is also growing.
Which aspect of teaching at your department you think deserves special mention?
We are trying to focus on practical learning. Medics appreciate that our occupational therapists train simulated disability with them, meaning that they for instance simulate a dysfunctional limb. I think this is an interesting experience and one that can help them in their future careers. It helps them appreciate what patients may be experiencing and what their problems are, including issues they may have failed to consider before. And by the way, we had a great success with this approach also among physicians training for certificate in rehabilitation medicine.
What research projects does your department work on at the moment?
I have always been especially interested in patients after a brain injury or stroke. These conditions are linked to spasticity, a symptom of central paresis, which can be quite challenging for many patients. This is why I also regularly work at the Department of Neurology of the General University Hospital, where I am in a team focused on the treatment of spasticity and where I administer injections of botulotoxin A in patients’ spastic muscles. Patients with spastic paresis are also treated by physiotherapists and occupational therapists, so their care is really comprehensive.
At our department, we are also trying to identify prognostic factors which would help us assess a likely future development and level of intensity of care a patient may need already at the beginning of treatment. Future development heads in the direction of accurate assessment of intensity of rehabilitation and relative representation of physiotherapy, occupational therapy, and particular rehabilitation methods. We are also interested in the relation between cognitive functions and the development of paresis or motoric functions. It is quite clear that patients with damaged cognitive functions do not understand what a physiotherapist or occupational therapist explains to them. They do not remember what they are supposed to do, and they are not motivated to work on their improvement because they have no overall understanding of their health status. We also believe it is important to assess patient’s progress over time, which is why we lobby for maximal implementation of the International Classification of Functional Abilities, Disability, and Health in healthcare. After all, even Professor Pfeiffer was member of the WHO team which developed this classification and thanks to Professor Švestková, our department is the only place in the Czech Republic where application of this classification system is taught.
Does your area of specialisation face any specific scientific challenges?
Rehabilitation after brain damage poses a number of challenges. For instance, scientists have for a long time searched for substances which could be administered during the initial phase of brain trauma to support plasticity of the central nervous system. This research, however, ran into a number of dead ends and it is unclear whether something new will be discovered. With respect to rehabilitation in general, the method of constraint-induced movement therapy is currently widely used, and we introduced it into the programme of our outpatient care centre. The main principle of this approach is that we immobilise patients’ healthy limb to force them to use an affected limb. In physiotherapy, current trends work with the use of robotic systems. So far, however, robots cannot replace people and their work. They represent rather an addition or an improvement.
Many researchers also focus on patients in a vegetative state or minimally conscious state and try to find out how one could influence their progress to full consciousness. In some cases, patients never wake, and we do not know why that is so, and it seems that this is not necessarily linked to damage of a particular part of the brain.
What should improve in rehabilitation medicine to further improve patient care in our country?
First of all, I would welcome some system changes regarding the organisation of rehabilitation. So far, we do not have enough rehabilitation centres with interdisciplinary teams that would have enough time and the right facilities to care for severely affected patients. The total amount of financial resources going to rehabilitation is perhaps not so small, but their distribution is wrong. We have critically little money for the acute stage in severely affected patients who would not have to remain in such a state if we had enough specialists who would work with them intensively.
Do you personally attend some rehabilitation or physiotherapy?
I must say that in my case, the old adage about the greatest darkness being under a candle is right. I know exactly what I should do, but forcing myself to actually do it, that is a problem! What I advise to patients, I advise to myself as well, but I do not listen. But when the going gets tough, I do my best.
How do you view sports from the perspective of your specialisation?
I believe people should do sports mainly for fun. I am not sure whether especially competitive sportsmen and sportswomen do not overdo their training to the detriment of their future health. I do understand they want to be best in something and the temptation of winning is great, but sometimes they seem to forget that each organism has only a limited capacity. If they exhaust this capacity at a relatively young age, they may have little left for later in life, after a career in sports, and that part of life tends to be much longer. But no young person wants to admit that one day, he or she will grow old :)
I occasionally do sports for fun. I like going to the mountains, both in winter and in the summer, when I mainly enjoy the nature. I ski, do a bit of biking, and I used to be very fond of dancing.
By the way, do you wear high heels?
To a limited extent. With some outfits they are important, and they make me feel good, but the older I get, the less I wear them and the more I prefer more comfortable shoes.
How do you relax?
I like relaxing with travel films. I also like going to theatre or concerts of classical music. I am also trying to travel but for that, I do not have as much time as I would like.
jat
Photo: Markéta Sýkorová
